
Weight Loss Blood Test
£105
Your sample goes to a UKAS accredited laboratory meeting ISO 15189 standards.
After you receive your order confirmation email, please reply with your date of birth.
Venous Blood Collection Kit
This kit is sent to you and taken to your chosen clinic. The phlebotomist will collect your sample using the materials provided.
- 1Vacutainer blood collection tubes
- 2Needle and butterfly needle
- 3Tourniquet
- 4Alcohol swab
- 5Cotton wool and gauze
- 6Adhesive plaster
- 7Biohazard specimen bag
- 8Prepaid return envelope (Royal Mail Tracked 24)
- 9Laboratory request form
- 10Instructions for the phlebotomist
Follicle Stimulating Hormone (FSH) is produced in the pituitary gland and is important for women in the production of eggs by the ovaries and for men in the production of sperm. In women, FSH stimulates the enlargement of follicles within the ovaries in the first half of the menstrual cycle. FSH levels rise significantly during perimenopause and menopause, which can affect body composition and make weight management more challenging. In men, FSH acts on the testicles to stimulate sperm production.
Oestradiol is the strongest of the three oestrogens and is produced in both the ovaries and testes. It's responsible for the growth of breast tissue, the female reproductive system, and male sexual function. In pre-menopausal women, oestradiol levels vary throughout the monthly cycle, peaking just before ovulation. Levels are lowest after menopause. Declining oestradiol during perimenopause and menopause can lead to changes in fat distribution, with increased abdominal fat storage. In men, oestradiol levels tend to increase with age as testosterone declines, which can contribute to weight gain and body composition changes.
Testosterone is a hormone that causes male characteristics and is produced in the testicles of men and, in much smaller amounts, in the ovaries of women. It helps regulate sex drive, bone mass, fat distribution, muscle mass, strength, and red blood cell production. Testosterone levels in men naturally decline after age 30. Low testosterone can make it harder to build and maintain muscle mass, which affects your metabolic rate and ability to burn calories. Symptoms include fatigue, difficulty gaining muscle, increased body fat (particularly around the abdomen), and low energy—all of which can impact weight management efforts.
Thyroid stimulating hormone (TSH) is produced by the pituitary gland to regulate the production of thyroid hormones thyroxine (T4) and triiodothyronine (T3) by the thyroid gland. If thyroid hormones in the blood are low, more TSH is produced to stimulate the thyroid gland. If thyroid hormone levels are high, the pituitary produces less TSH. An underactive thyroid (hypothyroidism) can cause weight gain, fatigue, and difficulty losing weight, while an overactive thyroid (hyperthyroidism) can cause weight loss. TSH is the most sensitive marker for detecting thyroid dysfunction and is often the first to change when thyroid problems develop.
Thyroxine (T4) is one of two hormones produced by the thyroid gland. It works to speed up the rate of your metabolism. Most T4 is bound to carrier proteins in the blood—it is only the free, or unbound, T4 that is active in the body, which is what this test measures. Free T4 is the less active of the two main thyroid hormones; it needs to convert to the more active T3 when your body needs it. Low free T4 levels, combined with high TSH, indicate an underactive thyroid which can significantly impact your ability to lose weight by slowing your metabolism.
Iron is a mineral essential for life. It is a component of haemoglobin, a protein in red blood cells responsible for transporting oxygen around the body. If you don't have enough iron, your haemoglobin levels fall and you can't get sufficient oxygen to your cells. This can cause symptoms including fatigue, dizziness, and shortness of breath—all of which can make it harder to exercise and stick to a weight loss programme. Serum iron is a transient reading and should be interpreted alongside other iron markers.
Total iron-binding capacity (TIBC) is a measure of the ability of your body to efficiently carry iron through the blood. TIBC is usually high when iron stores are low (iron deficiency) and low when iron stores are high (iron overload). It helps provide a fuller picture of your iron status alongside serum iron and ferritin.
Transferrin is made in the liver and is the major protein in the blood that binds to iron and transports it around the body. This test measures how much transferrin is 'saturated' by iron, expressed as a percentage. Low transferrin saturation indicates iron deficiency, while very high saturation can indicate iron overload. Normal saturation is typically 20–50%.
Ferritin is a protein that stores iron in your cells and tissues. Measuring ferritin gives a good indication of the amount of iron stored in your body. Low ferritin indicates depleted iron stores and can cause fatigue, weakness, and reduced exercise capacity—making weight loss efforts more difficult. Elevated ferritin can indicate inflammation, infection, or iron overload. Because ferritin is an acute phase reactant, it may be elevated during inflammation regardless of iron status.
Alanine transferase (ALT) is an enzyme mostly found in the liver. If the liver is damaged, ALT is released into the bloodstream. As ALT is predominantly found in the liver, it is usually an accurate marker for liver inflammation. Elevated ALT is commonly seen in non-alcoholic fatty liver disease (NAFLD), which is strongly associated with excess body weight and obesity. Weight loss is one of the most effective ways to improve liver health in people with NAFLD.
Alkaline phosphatase (ALP) is an enzyme found mainly in the liver and bones. Measuring ALP can indicate ongoing liver, gallbladder, or bone disease. Elevated ALP alongside elevated GGT suggests a liver or gallbladder problem. Gallstones are more common in people who are overweight or who lose weight rapidly.
Gamma GT, also known as gamma-glutamyl transferase (GGT), is a liver enzyme which is raised in liver and bile duct diseases. It is used alongside ALP to distinguish between bone or liver disease. GGT is also used to diagnose alcohol-related liver damage, as it is raised in 75% of long-term drinkers. Elevated GGT can also be seen in non-alcoholic fatty liver disease (NAFLD), which is associated with obesity and metabolic syndrome.
Bilirubin is a product of the breakdown of haemoglobin from red blood cells. It is removed from the body via the liver, stored and concentrated in the gallbladder, and secreted into the bowel. It is removed from your body through urine and faeces. Elevated bilirubin can indicate liver disease, bile duct obstruction, or increased red blood cell breakdown. Mildly elevated bilirubin with normal liver enzymes may indicate Gilbert's syndrome, a common and harmless genetic condition.
Cholesterol is an essential fat (lipid) in the body with important functions including building cell membranes and producing hormones. Cholesterol is manufactured in the liver and also comes from food. The two main components of total cholesterol are HDL (high-density lipoprotein), which is protective against heart disease, and LDL (low-density lipoprotein), which in high levels can contribute to cardiovascular disease. Being overweight is associated with higher cholesterol levels. As you lose weight, you'll typically see improvements in your cholesterol profile.
LDL cholesterol (low-density lipoprotein) is a molecule made of lipids and proteins which transports cholesterol, triglycerides, and other fats to various tissues throughout the body. Too much LDL cholesterol, commonly called 'bad cholesterol', can cause fatty deposits to accumulate inside artery walls, potentially leading to atherosclerosis and heart disease. Excess body weight, particularly visceral fat around the abdomen, is strongly associated with elevated LDL cholesterol levels.
HDL cholesterol (high-density lipoprotein) is a molecule that removes cholesterol from the bloodstream and transports it to the liver where it is broken down and removed from the body in bile. HDL cholesterol is commonly known as 'good cholesterol' because higher levels are protective against heart disease. Regular exercise and weight loss can help increase HDL cholesterol levels.
Non-HDL cholesterol is calculated by subtracting your HDL cholesterol from your total cholesterol. It includes all the non-protective and potentially harmful cholesterol in your blood, including LDL, VLDL (very low-density lipoproteins), and other lipoproteins thought to be even more harmful than LDL. As such, non-HDL cholesterol is considered a better marker for cardiovascular risk than total cholesterol or LDL alone. The recommended level is below 4 mmol/L.
The cholesterol: HDL ratio is calculated by dividing your total cholesterol value by your HDL cholesterol level. It is used as a measure of cardiovascular risk because it gives good insight into the proportion of your total cholesterol which is protective (HDL). Heart disease risk tools use this ratio to calculate your risk of having a heart attack. A lower ratio is better—ideally below 4 for men and below 3.5 for women.
Triglycerides are a type of fat (lipid) that circulates in the blood. After you eat, your body converts excess calories—whether from fat or carbohydrates—into triglycerides, which are then transported to cells to be stored as fat. Your body releases triglycerides when required for energy. High triglyceride levels are strongly associated with excess body weight, particularly abdominal obesity, and are a marker for metabolic syndrome. Reducing carbohydrate and alcohol intake, losing weight, and increasing physical activity can help lower triglyceride levels.
Haemoglobin A1c (HbA1c), also known as glycated haemoglobin, is a longer-term measure of glucose levels in your blood than a simple blood glucose test. Glucose attaches itself to the haemoglobin in your red blood cells, and as red cells live for around 12–16 weeks, it gives a good indication of the average sugar level in your blood over a 3-month period. A raised HbA1c result points to diabetes or an increased risk of developing diabetes (prediabetes). Insulin resistance and prediabetes can make weight loss significantly more difficult because your body becomes less efficient at using glucose for energy and more prone to storing it as fat, particularly around the abdomen.
Vitamin D (25 OH) is the major circulating form of vitamin D and is the most accurate indicator of vitamin D supply to your body. Vitamin D is essential for healthy bones and teeth, muscle health, immune function, and mental health. Low vitamin D symptoms include muscle weakness, mood swings, and fatigue—all of which can make it harder to exercise and maintain motivation for weight loss. People who are overweight or obese tend to have lower vitamin D levels because vitamin D is stored in fat tissue, making it less available to the body. Weight loss can help improve vitamin D levels.
High-sensitivity CRP (hs-CRP) is an inflammation marker used to detect low-level inflammation thought to damage blood vessels and increase heart disease risk. Excess body fat, particularly visceral fat around the abdomen, produces inflammatory compounds that raise hs-CRP levels. This chronic low-grade inflammation is associated with insulin resistance, metabolic syndrome, and cardiovascular disease. Weight loss typically results in lower hs-CRP levels and reduced inflammation throughout the body.
Cortisol is a stress hormone produced by the adrenal glands. It is vital to survival given its role in immunity, regulating blood pressure, and releasing insulin for blood sugar maintenance. However, chronically elevated cortisol—often due to ongoing stress—can promote weight gain, particularly around the abdomen (visceral fat). High cortisol increases appetite and cravings for high-calorie foods, promotes fat storage, and can break down muscle tissue, reducing your metabolic rate. Cortisol levels follow a daily rhythm, typically highest in the morning and lowest at night, which is why timing of the blood test is important.
This test is for screening and information only — it is not a medical diagnosis or professional advice. Please have your results reviewed by a qualified doctor or healthcare provider who can explain what they mean for your personal health situation. If your results show anything outside the normal range, or if you're worried about your health, see your doctor as soon as you can. Don't change any medications or treatments based on these results alone — always talk to your healthcare provider first.
NO CLINICS, NO QUEUES, NO HASSLE
Four steps to clarity
 01
01
Pick your panel
Browse over 200 clinically designed test kits and choose the one that fits your goals.
 02
02
Kit to your door
Everything you need arrives in discreet packaging with step-by-step instructions inside.
 03
03
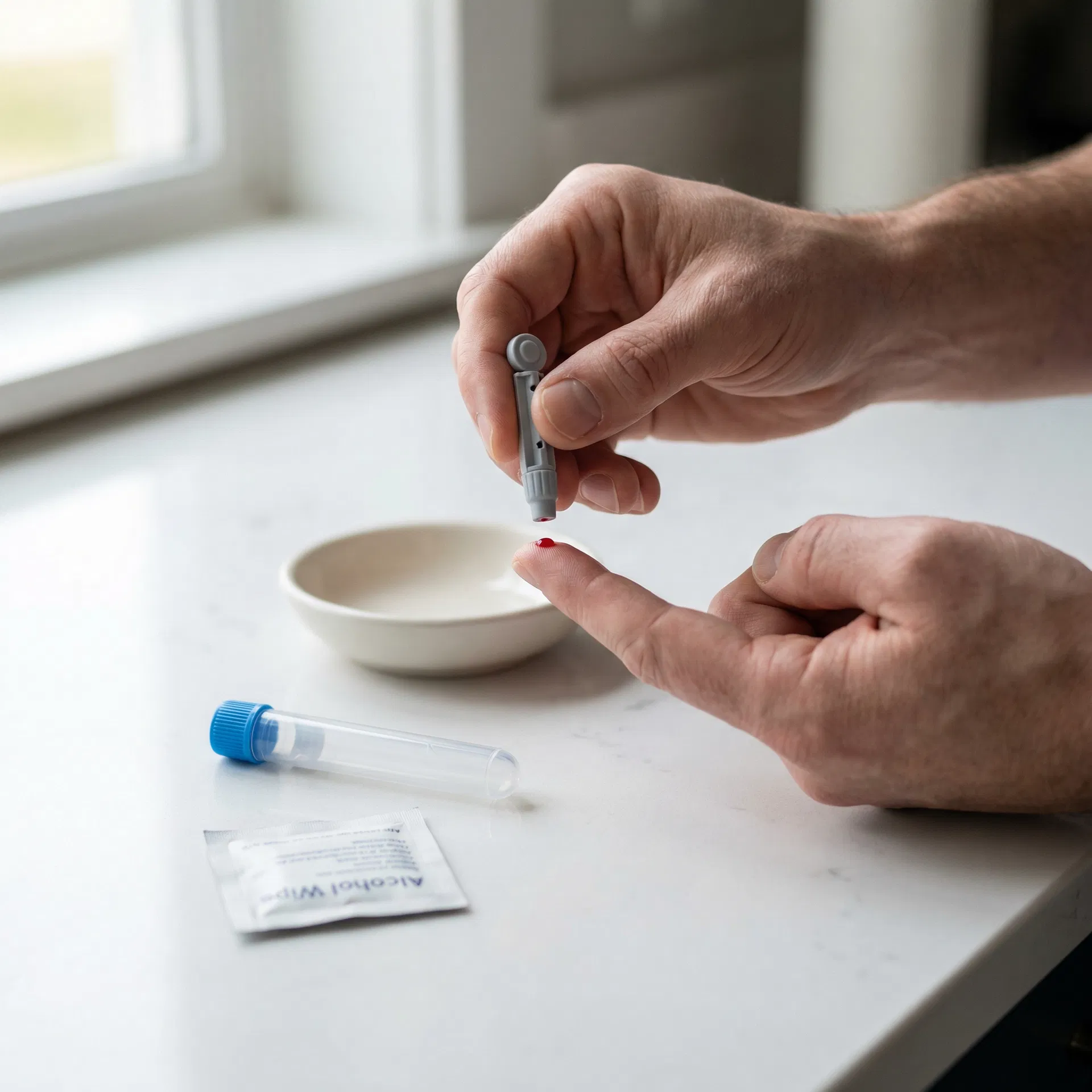
Collect your sample
Follow the simple instructions in your kit — whether it's a finger-prick at home or a venous draw at a partner clinic.
 04
04
Insights delivered
Clear, easy-to-understand results sent to you online with actionable health guidance.
Frequently asked questions
Your kit includes a single-use lancet device. Clean your finger with the provided wipe, prick your fingertip, and fill the collection tube to the line indicated. Full step-by-step instructions are included in your kit.
Results are typically available within 2 working days of your sample reaching our UKAS accredited laboratory. You will receive an email notification when your results are ready.
If any of your results fall outside the normal range, we recommend booking an appointment with your GP to discuss them. Our results include reference ranges and guidance.
Unless specifically stated in your test instructions, fasting is not required. Check the product description for any specific preparation requirements for this test.
