
Menopause Blood Test Kit
£68
Your sample goes to a UKAS accredited laboratory meeting ISO 15189 standards.
After you receive your order confirmation email, please reply with your date of birth.
Venous Blood Collection Kit
This kit is sent to you and taken to your chosen clinic. The phlebotomist will collect your sample using the materials provided.
- 1Vacutainer blood collection tubes
- 2Needle and butterfly needle
- 3Tourniquet
- 4Alcohol swab
- 5Cotton wool and gauze
- 6Adhesive plaster
- 7Biohazard specimen bag
- 8Prepaid return envelope (Royal Mail Tracked 24)
- 9Laboratory request form
- 10Instructions for the phlebotomist
Follicle-stimulating hormone (FSH) is produced by the pituitary gland and plays a central role in reproduction. In premenopausal women, FSH stimulates the development of ovarian follicles (fluid-filled sacs containing eggs) during the first half of the menstrual cycle. As follicles mature, they produce increasing amounts of oestradiol. A "feedback loop" exists: when oestradiol rises sufficiently, it signals the pituitary to reduce FSH production. After ovulation, FSH levels fall and remain low during the second half of the cycle. As women approach menopause, the ovaries contain fewer remaining follicles and become less responsive to FSH. The pituitary gland responds by producing more and more FSH in an attempt to stimulate the ovaries—like turning up the thermostat when the heating isn't working. This is why FSH levels rise during perimenopause and menopause. Measuring FSH on day 2-5 of the menstrual cycle provides the most reliable assessment; at other times, levels naturally fluctuate. In premenopausal women (day 2-5), FSH is typically 3-10 IU/L. During perimenopause, FSH begins to rise and often fluctuates unpredictably—it may be elevated one month and normal the next. Persistently elevated FSH above 25-40 IU/L, particularly when combined with low oestradiol and menstrual changes, suggests the menopausal transition is well underway or complete. FSH above 30-40 IU/L with amenorrhoea (no periods) for 12 months is consistent with menopause. However, a single FSH measurement cannot definitively "diagnose" menopause—the perimenopause is characterised by hormonal variability, and repeat testing may be needed. Results outside the normal range may need a follow-up with your GP.
Luteinising hormone (LH) is produced by the pituitary gland and works alongside FSH to regulate the menstrual cycle and ovulation. In premenopausal women, LH levels remain relatively low during most of the cycle but surge dramatically mid-cycle—this "LH surge" triggers ovulation (the release of a mature egg from the ovary). After ovulation, LH stimulates the empty follicle to become the corpus luteum, which produces progesterone to prepare the uterine lining for potential pregnancy. Like FSH, LH levels rise during perimenopause and menopause as the pituitary attempts to stimulate the increasingly unresponsive ovaries. However, LH typically rises later than FSH and to a lesser degree, so FSH is generally considered the more sensitive marker of ovarian reserve and menopausal status. The FSH: LH ratio can provide additional information—in reproductive-age women, FSH and LH are usually similar (ratio ~1:1), while in menopause, FSH typically exceeds LH. In premenopausal women (day 2-5), LH is typically 2-10 IU/L (with a mid-cycle surge to 20-100+ IU/L during ovulation). During perimenopause and menopause, baseline LH rises, typically to 15-60 IU/L. The LH: FSH ratio can sometimes help distinguish menopause from other conditions—for example, in polycystic ovary syndrome (PCOS), LH is often elevated relative to FSH (ratio 2:1 or 3:1), whereas in menopause FSH is typically higher than or equal to LH. LH is interpreted alongside FSH and oestradiol for a complete picture. Results outside the normal range may need a follow-up with your GP.
Oestradiol (also spelled estradiol, often abbreviated as E2) is the most potent and abundant oestrogen in premenopausal women. It's produced primarily by the ovarian follicles and is responsible for the development and maintenance of female reproductive tissues, breast development, bone health, cardiovascular protection, skin health, and cognitive function. Oestradiol also affects mood, sleep, and libido. In premenopausal women, oestradiol levels vary dramatically across the menstrual cycle—lowest at the start of the cycle, rising as follicles develop, peaking just before ovulation, then fluctuating in the second half. During perimenopause, oestradiol levels become erratic. Early perimenopause may actually see higher-than-normal oestradiol levels on some days as the pituitary pumps out FSH and stimulates remaining follicles. Later perimenopause typically sees declining and inconsistent oestradiol. After menopause, the ovaries essentially stop producing oestradiol, and levels drop to very low—typically below 100 pmol/L (or <30 pg/mL). This dramatic oestrogen decline is responsible for most menopausal symptoms including hot flushes, night sweats, vaginal dryness, sleep disturbances, and accelerated bone loss. In premenopausal women (day 2-5), oestradiol is typically 100-400 pmol/L (30-120 pg/mL). It rises mid-cycle to 400-1500 pmol/L (120-450 pg/mL) around ovulation. In postmenopausal women not on HRT, oestradiol is typically below 100 pmol/L (<30 pg/mL). The combination of high FSH with low oestradiol is the classic hormonal pattern of menopause. If oestradiol is still elevated, it may mask a high FSH reading (because oestradiol suppresses FSH), so both markers together give a more accurate picture than either alone. Results outside the normal range may need a follow-up with your GP.
Thyroid-stimulating hormone (TSH) is produced by the pituitary gland and controls the thyroid gland's production of thyroid hormones (T4 and T3). TSH works through a feedback mechanism: when thyroid hormone levels drop, the pituitary releases more TSH to stimulate the thyroid; when thyroid hormone levels rise, TSH production decreases. This makes TSH the most sensitive marker of thyroid function—abnormal TSH is usually the first sign of thyroid dysfunction. Thyroid disorders are significantly more common in women than men and often emerge or worsen around the time of menopause. Importantly, hypothyroidism (underactive thyroid) causes symptoms that closely mimic menopause: fatigue, weight gain, cold intolerance, dry skin, hair thinning, constipation, low mood, and brain fog. Hyperthyroidism (overactive thyroid) can cause anxiety, palpitations, heat intolerance, and irregular periods—also potentially confused with perimenopause. This overlap makes checking thyroid function essential when investigating menopausal symptoms. Normal TSH is typically 0.4-4.0 mIU/L, though many laboratories use narrower optimal ranges (0.5-2.5 mIU/L). Elevated TSH (above 4.0-4.5 mIU/L) suggests hypothyroidism—the thyroid isn't producing enough hormone, so the pituitary makes more TSH trying to stimulate it. Low TSH (below 0.4 mIU/L) suggests hyperthyroidism—excess thyroid hormone is suppressing TSH production. Subclinical thyroid disease (mildly abnormal TSH with normal free T4) is common and may still cause symptoms. If your TSH is abnormal, further investigation and treatment may significantly improve your symptoms. Results outside the normal range may need a follow-up with your GP.
Free T4 (free thyroxine) measures the amount of unbound, biologically active thyroxine circulating in your blood. The thyroid gland produces thyroxine (T4) as its primary hormone. Most T4 in the blood is bound to carrier proteins and is inactive; only the small "free" fraction (about 0.03% of total T4) is available to enter cells and exert biological effects. T4 itself is relatively inactive—it's converted to the more active T3 (triiodothyronine) in tissues throughout the body as needed. Free T4 is measured alongside TSH to confirm and characterise thyroid dysfunction. In primary hypothyroidism (thyroid gland failure), TSH is elevated and free T4 is low—the thyroid simply can't produce enough hormone despite being stimulated. In primary hyperthyroidism (overactive thyroid), TSH is suppressed and free T4 is elevated—excess hormone production is shutting down the pituitary's TSH output. In subclinical thyroid disease, TSH is abnormal but free T4 remains within the normal range. Normal free T4 is typically 9-25 pmol/L (0.7-1.9 ng/dL), though ranges vary between laboratories. Low free T4 with elevated TSH confirms hypothyroidism. Low free T4 can cause fatigue, weight gain, cold intolerance, constipation, dry skin, and depression—symptoms that overlap significantly with menopause. High free T4 with suppressed TSH confirms hyperthyroidism, which can cause anxiety, tremor, palpitations, weight loss, and heat intolerance. Identifying thyroid dysfunction is important because it's readily treatable—levothyroxine for hypothyroidism, various options for hyperthyroidism—and treatment can dramatically improve quality of life. Results outside the normal range may need a follow-up with your GP.
This test is for screening and information only — it is not a medical diagnosis or professional advice. Please have your results reviewed by a qualified doctor or healthcare provider who can explain what they mean for your personal health situation. If your results show anything outside the normal range, or if you're worried about your health, see your doctor as soon as you can. Don't change any medications or treatments based on these results alone — always talk to your healthcare provider first.
NO CLINICS, NO QUEUES, NO HASSLE
Four steps to clarity
 01
01
Pick your panel
Browse over 200 clinically designed test kits and choose the one that fits your goals.
 02
02
Kit to your door
Everything you need arrives in discreet packaging with step-by-step instructions inside.
 03
03
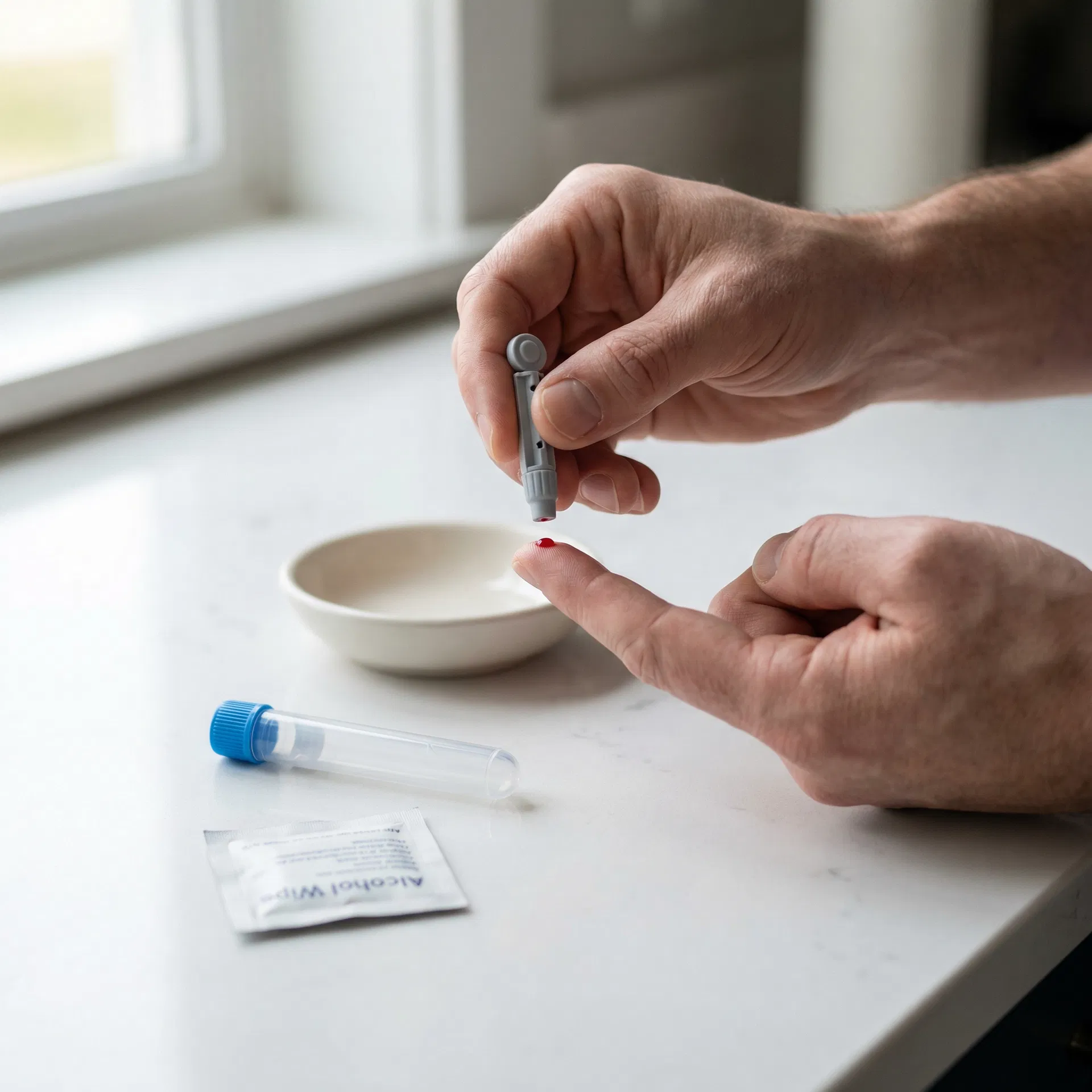
Collect your sample
Follow the simple instructions in your kit — whether it's a finger-prick at home or a venous draw at a partner clinic.
 04
04
Insights delivered
Clear, easy-to-understand results sent to you online with actionable health guidance.
Frequently asked questions
Your kit includes a single-use lancet device. Clean your finger with the provided wipe, prick your fingertip, and fill the collection tube to the line indicated. Full step-by-step instructions are included in your kit.
Results are typically available within 2 working days of your sample reaching our UKAS accredited laboratory. You will receive an email notification when your results are ready.
If any of your results fall outside the normal range, we recommend booking an appointment with your GP to discuss them. Our results include reference ranges and guidance.
Unless specifically stated in your test instructions, fasting is not required. Check the product description for any specific preparation requirements for this test.
