Female Infertility Check Blood test
£60 ✓ In Stock
Your sample goes to a UKAS accredited laboratory meeting ISO 15189 standards.
After you receive your order confirmation email, please reply with your date of birth.
How it works
Your testing journey
From order to results in four simple steps. Full transparency on where each step happens and what it costs.

Receive your kit by post
Dispatched same working day if ordered before 3pm. Royal Mail Tracked delivery, typically 1–3 working days. 90% of kits arrive within 24 hours.

Visit a partner clinic
Book a phlebotomy appointment at one of our 365+ UK partner clinics. Take your kit with you — the phlebotomist will collect your sample using the materials provided.
Phlebotomy fee applies (paid at clinic)
Venous blood draw at a clinic
A trained phlebotomist takes a small blood sample from a vein in your arm using the vacutainers provided in your kit. The appointment takes around 10 minutes.

Return by prepaid envelope
Seal your sample in the biohazard bag provided and drop it in any Royal Mail postbox using the prepaid Tracked 24 envelope. Post Monday–Thursday for best results.
Venous Blood Collection Kit
This kit is sent to you and taken to your chosen clinic. The phlebotomist will collect your sample using the materials provided.
- 1Vacutainer blood collection tubes
- 2Needle and butterfly needle
- 3Tourniquet
- 4Alcohol swab
- 5Cotton wool and gauze
- 6Adhesive plaster
- 7Biohazard specimen bag
- 8Prepaid return envelope (Royal Mail Tracked 24)
- 9Laboratory request form
- 10Instructions for the phlebotomist
Follicle Stimulating Hormone (FSH) is produced by the pituitary gland in the brain and plays a crucial role in female reproduction. As its name suggests, FSH stimulates the growth and development of ovarian follicles—the fluid-filled sacs in the ovaries that contain eggs. Each month, FSH prompts several follicles to begin developing, and as they grow, they produce oestradiol. Eventually, one follicle becomes dominant and releases a mature egg at ovulation. Baseline FSH levels (measured on day 2-3 of the menstrual cycle) are one of the most commonly used markers of ovarian reserve—an indication of how many eggs remain in your ovaries and how well they may respond to stimulation. The feedback loop works like this: when ovarian reserve is good and follicles respond readily to FSH, the ovaries produce adequate oestradiol, which signals the pituitary to keep FSH production moderate. When ovarian reserve is diminished and follicles respond less well, the pituitary compensates by producing more FSH—essentially "stepping on the gas" to try to stimulate the remaining follicles. Normal day 2-3 FSH levels are typically between 3-10 IU/L. Levels above 10 IU/L may suggest reduced ovarian reserve, and levels above 15-20 IU/L often indicate significantly diminished reserve. However, FSH must be interpreted alongside oestradiol (a high oestradiol can artificially suppress FSH, masking reduced reserve) and in the context of your age—ovarian reserve naturally declines with age, and a given FSH level means different things at 28 versus 42. Persistently elevated FSH above 25-40 IU/L, combined with absent periods and low oestradiol, is consistent with menopause or premature ovarian insufficiency. Results outside the normal range may need a follow-up with your GP or a fertility specialist.
Luteinising Hormone (LH) is produced by the pituitary gland and works alongside FSH to regulate the menstrual cycle and ovulation. While FSH stimulates follicle growth in the first half of the cycle, LH triggers ovulation—the release of a mature egg from the dominant follicle. The dramatic surge in LH that occurs mid-cycle (the "LH surge") is what home ovulation predictor kits detect. After ovulation, LH also stimulates the empty follicle to transform into the corpus luteum, which produces progesterone to support early pregnancy. Baseline LH levels (measured on day 2-3) are typically similar to or slightly lower than FSH, usually between 2-10 IU/L. The ratio of LH to FSH provides additional diagnostic information. In healthy women, the LH: FSH ratio is typically around 1:1 or slightly less. An elevated LH: FSH ratio (often 2:1 or 3:1) is characteristic of polycystic ovary syndrome (PCOS), one of the most common causes of anovulatory infertility. In PCOS, tonically elevated LH disrupts the normal hormonal signalling needed for regular ovulation. Very low LH levels may indicate a problem with the pituitary gland or hypothalamus (hypothalamic amenorrhoea), which can occur with extreme weight loss, excessive exercise, or severe stress. Like FSH, persistently elevated LH combined with absent periods may indicate menopause or premature ovarian insufficiency. Results should be interpreted alongside FSH, oestradiol, and your clinical picture. Results outside the normal range may need a follow-up with your GP or a fertility specialist.
Oestradiol (also spelled estradiol, abbreviated E2) is the most potent form of oestrogen and the primary oestrogen produced by the ovaries during reproductive years. It's produced by the granulosa cells of developing ovarian follicles in response to FSH stimulation. Oestradiol levels rise as follicles develop during the first half of the menstrual cycle (follicular phase), peak just before ovulation, drop briefly, then rise again during the second half (luteal phase) before falling to trigger menstruation if pregnancy doesn't occur. Baseline oestradiol (measured on day 2-3) should be relatively low—typically below 200 pmol/L (or approximately 55 pg/mL). If oestradiol is elevated early in the cycle, this may indicate an ovarian cyst, early follicle recruitment, or declining ovarian reserve. Importantly, an elevated baseline oestradiol can artificially suppress FSH levels, making FSH appear normal when ovarian reserve is actually diminished. This is why oestradiol and FSH should always be interpreted together. Very low oestradiol levels combined with elevated FSH indicate ovarian insufficiency or menopause—the ovaries are no longer producing adequate oestrogen despite high FSH stimulation. Low oestradiol with low FSH and LH suggests a problem at the level of the pituitary or hypothalamus (hypogonadotropic hypogonadism). Normal oestradiol with an elevated LH: FSH ratio may be seen in PCOS. Oestradiol is also important beyond fertility—adequate levels are needed for bone health, cardiovascular protection, and general wellbeing. Results outside the normal range may need a follow-up with your GP or a fertility specialist.
Prolactin is a hormone produced primarily by the pituitary gland. Its main function is to stimulate breast milk production after childbirth, but it also plays important roles in reproductive function even outside of pregnancy and breastfeeding. In non-pregnant, non-breastfeeding women, prolactin levels should be relatively low—typically below 500-600 mU/L (or approximately 25 ng/mL, depending on the assay). Elevated prolactin (hyperprolactinaemia) is an important and treatable cause of infertility. High prolactin suppresses the release of GnRH (gonadotropin-releasing hormone) from the hypothalamus, which in turn reduces FSH and LH secretion from the pituitary. This disrupts the normal hormonal signals needed for follicle development and ovulation. Women with hyperprolactinaemia may experience irregular periods, absent periods (amenorrhoea), milky nipple discharge (galactorrhoea) even without pregnancy, and difficulty conceiving. The most common cause of significantly elevated prolactin is a prolactinoma—a benign (non-cancerous) tumour of the pituitary gland that secretes prolactin. Fortunately, prolactinomas are usually easily treated with medication (dopamine agonists like cabergoline or bromocriptine), which can normalise prolactin levels, restore ovulation, and allow conception. Other causes of elevated prolactin include certain medications (particularly some antipsychotics and anti-nausea drugs), hypothyroidism, and sometimes PCOS. Mildly elevated prolactin can also result from stress, recent nipple stimulation, or blood sampling conditions—this is why morning sampling after rest is important. If prolactin is elevated, repeat testing and further investigation (possibly including pituitary imaging) is usually recommended. Results outside the normal range may need a follow-up with your GP or an endocrinologist.
This test is for screening and information only — it is not a medical diagnosis or professional advice. Please have your results reviewed by a qualified doctor or healthcare provider who can explain what they mean for your personal health situation. If your results show anything outside the normal range, or if you're worried about your health, see your doctor as soon as you can. Don't change any medications or treatments based on these results alone — always talk to your healthcare provider first.
NO CLINICS, NO QUEUES, NO HASSLE
Four steps to clarity
 01
01
Pick your panel
Browse over 200 clinically designed test kits and choose the one that fits your goals.
 02
02
Kit to your door
Everything you need arrives in discreet packaging with step-by-step instructions inside.
 03
03
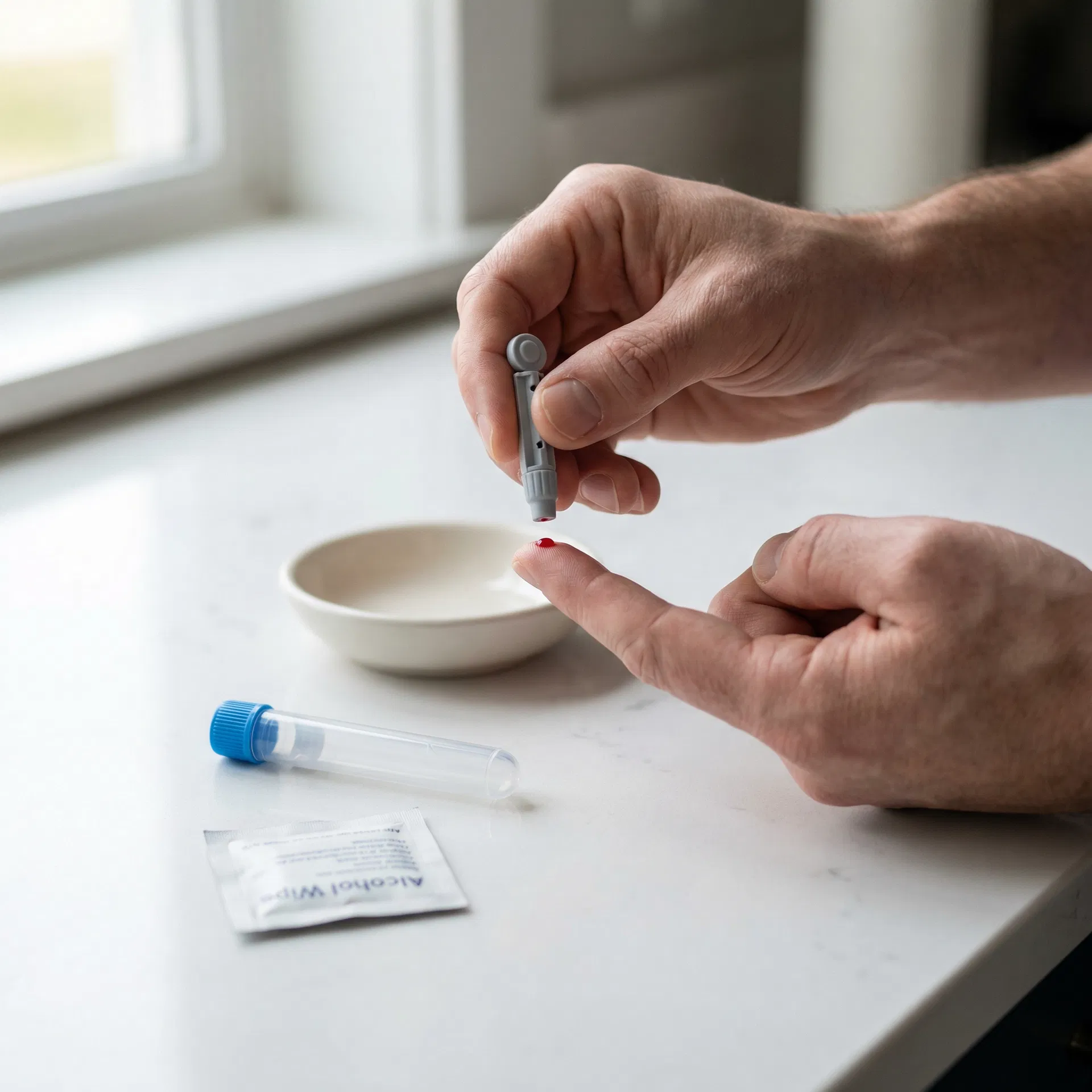
Collect your sample
Follow the simple instructions in your kit — whether it's a finger-prick at home or a venous draw at a partner clinic.
 04
04
Insights delivered
Clear, easy-to-understand results sent to you online with actionable health guidance.
Frequently asked questions
This test measures FSH (Follicle Stimulating Hormone), LH (Luteinising Hormone), Oestradiol (E2), Prolactin. Check the full biomarker list on this page for detailed descriptions of each marker and what it tells you about your health.
Check the Special Instructions section on this page. As a general rule, if the panel includes cholesterol, triglycerides, glucose, or insulin, fast for 8-12 hours. For most hormone, vitamin, and antibody tests, fasting is not required. Morning collection (7-10am) is preferred.
Follow the instructions in your kit. For finger-prick tests: warm your hands, use the lancet as directed, fill the tube to the marked line. For venous tests: attend a phlebotomy clinic with your laboratory request form. Post your sample the same day — avoid Fridays and bank holidays.
Results are typically available within the timeframe shown on this page. You will receive a notification when ready to view online. Results include reference ranges and guidance.




